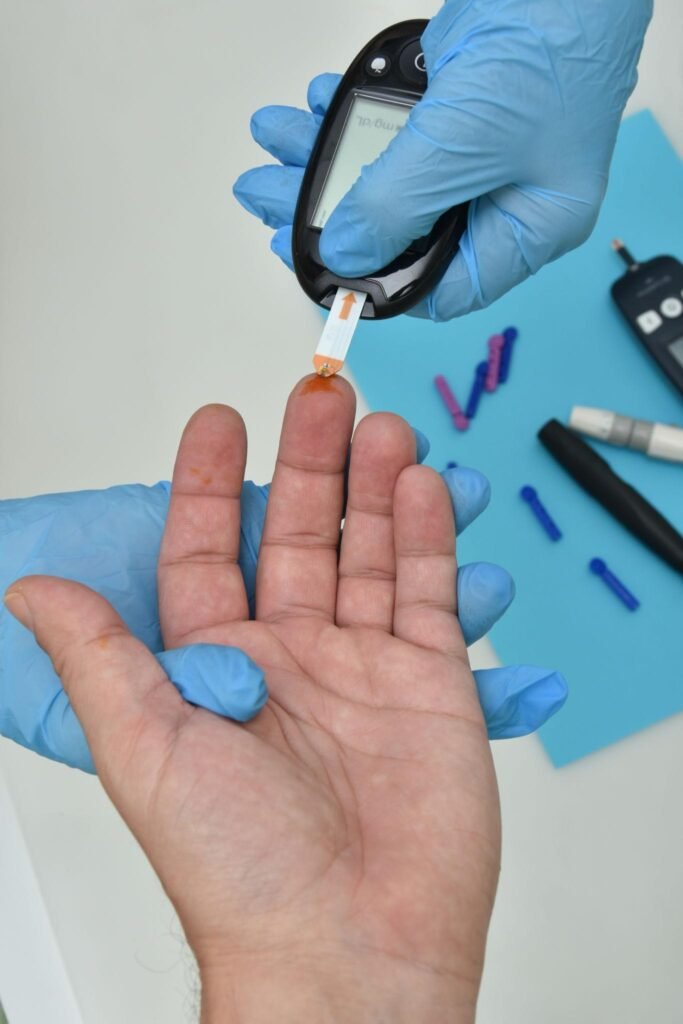



Jardiance (empagliflozin) is a modern oral medication widely used in the treatment of type 2 diabetes and increasingly in cardiovascular and renal care. As part of the sodium-glucose co-transporter 2 (SGLT2) inhibitor class, it represents a shift from traditional glucose-lowering therapies by targeting kidney function rather than insulin pathways.
Its growing use in clinical practice reflects not only its effectiveness in controlling blood sugar but also its broader impact on long-term health outcomes.
What Jardiance Is Used For
Jardiance is prescribed for multiple indications, including:
- Type 2 diabetes mellitus
- Reduction of cardiovascular risk in patients with heart disease
- Support of kidney function in certain chronic conditions
Unlike some older diabetes medications, Jardiance addresses both metabolic control and organ protection.
For a practical overview of how it is used in real-world settings, including dosage and key details, see this guide on how Jardiance (empagliflozin) tablets are used in treatment:
jardiance empagliflozin tablets overview
Mechanism of Action
Jardiance works by inhibiting the SGLT2 protein located in the proximal tubules of the kidneys. This protein is responsible for reabsorbing glucose back into the bloodstream.
By blocking this process:
- Excess glucose is excreted in urine
- Blood glucose levels decrease
- Caloric loss may contribute to modest weight reduction
This insulin-independent mechanism makes Jardiance particularly useful for patients with insulin resistance.
Additional Cardiovascular and Renal Benefits
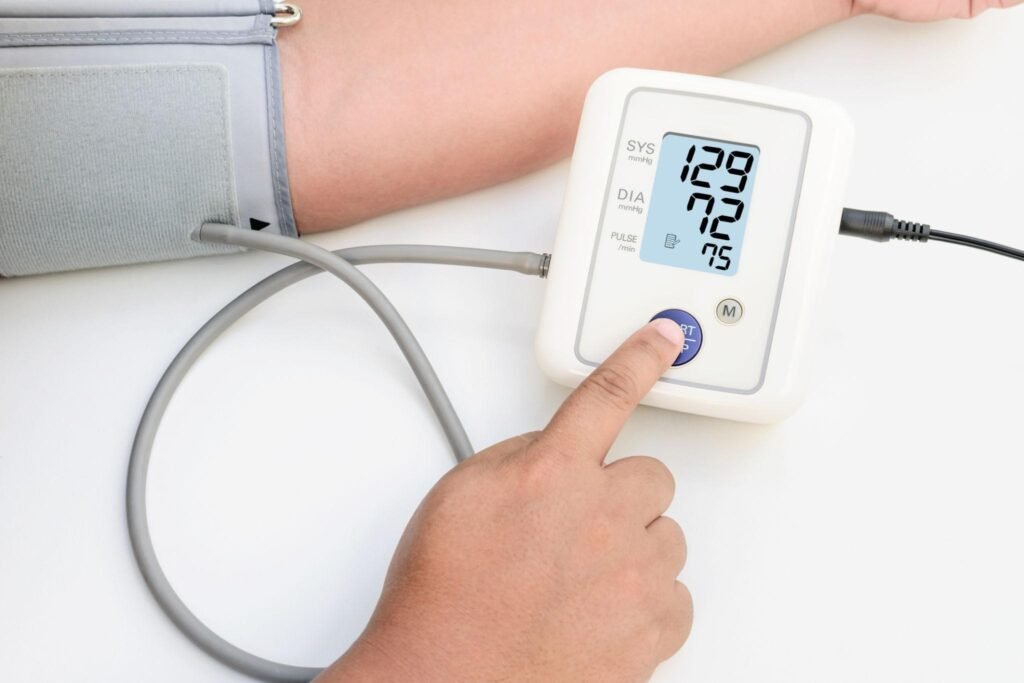



One of the most significant advantages of empagliflozin is its effect beyond glycemic control.
Clinical observations show that it may:
- Reduce the risk of hospitalization for heart failure
- Lower cardiovascular mortality in high-risk patients
- Slow progression of chronic kidney disease
These benefits have led to its inclusion in modern treatment guidelines for both endocrinology and cardiology.
Dosage and Administration
Jardiance is typically taken once daily:
- Starting dose: 10 mg per day
- May be increased depending on patient response
- Can be taken with or without food
Consistency is essential—taking the medication at the same time each day helps maintain stable blood levels.
Patients are also advised to stay hydrated, as the medication increases glucose excretion through urine.
Who Can Benefit Most
Jardiance may be particularly beneficial for:
- Patients with type 2 diabetes and cardiovascular risk factors
- Individuals with heart failure
- Patients with early-stage kidney disease
It is often used as part of combination therapy alongside other antidiabetic medications.
Potential Side Effects
While generally well tolerated, Jardiance may cause:
- Increased urination
- Urinary tract infections
- Genital infections
- Mild dehydration
In rare cases, more serious complications such as ketoacidosis may occur, especially in patients with specific risk factors.
Important Safety Considerations
Patients should consult a healthcare provider before starting Jardiance, particularly if they have:
- Kidney impairment
- Low blood pressure
- A history of recurrent infections
Regular monitoring of kidney function and hydration status is recommended during treatment.
For medically reviewed information on how empagliflozin works and its safety profile, see this clinical overview of empagliflozin mechanism and safety:
empagliflozin clinical mechanism and safety
Practical Tips for Best Results
To maximize the benefits of Jardiance:
- Take it consistently at the same time each day
- Maintain proper hydration
- Combine with a balanced diet and physical activity
- Follow regular medical check-ups
These steps improve both effectiveness and safety.
Conclusion
Jardiance (empagliflozin) is more than a standard diabetes medication—it is a multifunctional therapy that supports blood sugar control, heart health, and kidney function. Its unique mechanism and broad clinical benefits make it an important part of modern treatment strategies.
When used correctly and under medical supervision, it can significantly improve long-term outcomes for patients with chronic metabolic conditions.



